Non-Surgical Endodontics
Endodontic Procedure:
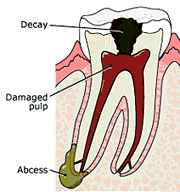
Endodontic treatment is necessary when the pulp becomes inflamed or infected. The inflammation or infection can be due to a variety of causes: deep decay, repeated dental procedures on the tooth, or a crack or chip in the tooth or traumatic injury to the tooth. If pulp inflammation or infection is left untreated, it can cause pain or lead to an abscess.
Signs of pulp damage include throbbing pain, prolonged sensitivity to heat or cold, discoloration of the tooth, swelling and tenderness in the nearby gum. Sometimes, there are no symptoms.
Endodontic treatment can often be performed in one or two visits depending on the complexity of the canal system and the severity of the infection. It involves the following steps:
1) We examine and perform several tests to determine the pulpal status, x-ray the tooth, then administers local anesthesia. After the tooth is numb, a small protective sheet called a "dental dam" is placed over the area to isolate the tooth and keep it clean and free of saliva during the procedure.
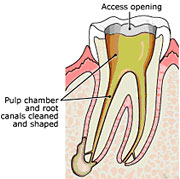
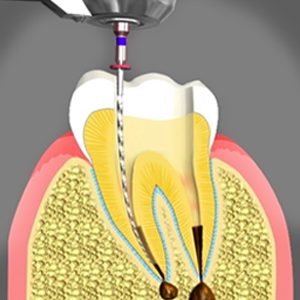
2) Then we make an opening in the crown of the tooth to get to the pulp chamber and locate the root canals. Anterior teeth and lower bicuspids usually have one canal, upper bicuspids usually have two canals and the molars have 3-5 canals. Very small instruments called files are used sequentially to clean and shape the canal system to receive the canal filling.
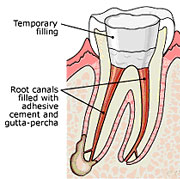
3) After the space is cleaned and shaped, the root canals are filled with a biocompatible material, usually a rubber-like material called "gutta-percha." The gutta-percha is placed with an adhesive cement to ensure complete sealing of the root canals. In most cases, a temporary filling is placed to close the opening. The temporary filling will be removed before the tooth is permanently restored.
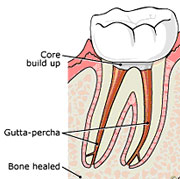
4) After the root canal is completed a crown or other restoration is placed on the tooth to protect and restore it to full function.
 General Dentistry
General Dentistry
 Invisalign
Invisalign
 Tooth Whitening
Tooth Whitening
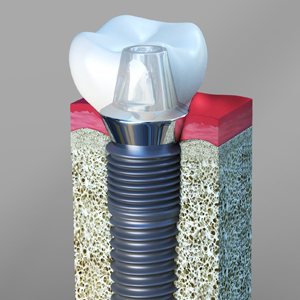 Dental Implants
Dental Implants
 Root Canals
Root Canals
 Other Services
Other Services